This biography is based on an interview with Jennifer Wilson in 2016 for the Early Medical Women of New Zealand Project. The interviewer was Claire Gooder.
Contents
Early years: the importance of an education
Jennifer Colston Wilson was born in Te Kuiti in 1934, the youngest daughter of Mabel Rose and Norman Edgar Wilson. Jenny and her older sisters Meredyth and Florence were all born at home, which later horrified Jenny when she developed an aversion to home births during her years training as an obstetrician.
Jenny’s mother Mabel was a graduate from the University of New Zealand (Auckland) and had a double MA in Art and History. She had taught at Opotiki School where she met Norman who was the son of the Headmaster, Henry Wilson. Norman had served in WW1 and been awarded the Military Cross. Mabel went back to work as a primary school teacher when Jenny was 7 years old, and this attitude towards women’s rights and education inspired her youngest daughter.
“She influenced me in this way, she told me that education was the most important thing in your life, that if you didn’t get educated, and you got married, that your husband could desert you, and your husband could die, and you needed to be educated to look after yourself on your own.”
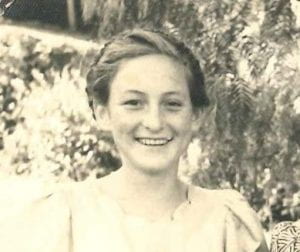
Jenny took her mother’s advice. At the age of 15, her family moved to Auckland, where Jenny entered Takapuna Grammar School at the lower sixth level. Within a few months she had risen to the top student in her new class. She was particularly inspired by one of her teachers, R.A. Scott, and it was his brilliance that allowed her to excel in physics and chemistry, and then eventually apply for medical school.
University: the motivation not to study medicine
Despite her academic potential, Jenny was initially hesitant to study medicine. She had witnessed her older sister Meredyth battle her way through medical school over eight years, and neither Jenny nor her mother felt that the experience should be repeated. Nonetheless, Jenny enrolled in medical intermediate in 1952, telling herself that if she didn’t pass the year, she would do a Bachelor of Science instead. However, Jenny excelled in her studies, and was the top student accepted into medical school.
“During that year I’d had appendicitis and I’d been off for three weeks, so it was quite an amazing thing to come top of the class.”
Jenny took the two-day long trip from Auckland to Otago Medical School via multiple trains and a boat ride. Compared to her medical intermediate year, which she had found particularly enjoyable, Jenny was less impressed with her first year in Otago. Her initial impression of Dunedin was ‘cold and dismal’, and she disliked the noisy environment of St Margaret’s hostel. Jenny suffered from periods of homesickness throughout her medical school training, and once went home during study break to visit her mother which was costly.
“When we did medical intermediate in Auckland it was great fun, it was me and about thirteen men. We all used to have lunch together, and it was a great deal of fun.”
“I hated the discipline of St Margaret’s. We had to be in the hostel by ten o’clock at night and we weren’t allowed out, and there were all sorts of restrictions. I hated it… The university clock—that was a very big challenge to me, it used to ring all night, you know, ding dong ding dong, you’re not asleep, ding dong ding dong, you’re not asleep. And it really interfered… I was quite neurotic about having to have enough sleep because I found that when I didn’t have enough sleep then my results were bad.”
Jenny was one of ten women in her medical school year. She was friendly with the other women, although she didn’t have many close friends. In her fifth year, Jenny moved out of the hostel and flatted with another medical school student—Patricia Clarkson—who was a lot of fun to live with.
The attitudes towards women in medical school were challenging for Jenny. She found the environment ‘frosty’, as women were expected to conform to the usual medical school norms, such as sitting in the front row, and working separately from the boys during anatomy dissections. Some of the teachers were particularly bossy, or sexist towards women.
“I think they were pretty disparaging, they told us we’re all going to get married and have kids and it would be a waste of time training us.”
However, Jenny did not let her gender get in the way of her studies. She was a very good student who was often top of her class, and as her training progressed, Jenny found her medical training more enjoyable. In particular, she appreciated being able to work with the male students during her fifth year training in Queen Mary Hospital. She was often in the company of her friend, Gerald Wong, and the two would sit together for their oral exams. In her final year she returned to Auckland for her practical training, where she was able to live in mixed accommodation within the hospital. Here she enjoyed socialising with others far more than she had in Dunedin.
Early career: the hard work, and the inspiration from mentors
After graduation, Jenny continued working in hospitals in Auckland for about three years, gaining experience in different specialties. The junior doctors were rotated around the different departments every three months, and the workload was challenging.
“I used to get tired when I was doing the jobs, because they were hard… I’d just have to go and lie down and have a sleep. I was in Auckland Hospital and you could do that.”
However, Jenny did not mind the hard work, she loved the hospital environment, and she was grateful to be on such a privileged career path. She was also fortunate to work with several brilliant mentors during her years as a house surgeon—including Dr Harvey Carey, Professor Liley, and Professor Herb Green—who inspired her choice to study obstetrics and gynaecology.
“Professor Carey had a marked effect on my training to be an obstetrician and gynaecologist. And then there was Professor Herb Green, which if you mention his name everybody gets hysterical, because he didn’t treat some women with pre-cancer of the cervix and some ended up with cancer. But he did do some other very good work, he stopped women having to have hysterectomies from abnormal smears. So that was a thing that people forget about.”
During the early years of her career, Jenny was the first woman to win the prestigious Doris Gordon Obstetrics and Gynaecology Travelling Scholarship. Rather than moving overseas as was the conventional route, she instead gained special permission to complete her study in New Zealand before later heading overseas with the intention of training in a London teaching hospital.
Family life: specialist challenges for a mother in medicine
Jenny met her future husband Trevor—also a medical student—during her sixth-year training in Auckland hospital. The couple were married shortly after graduation.
“I was a very shy girl and I think that that probably influenced my socialising. But in fifth year I had a good time. And I met my husband in the sixth year, he was at Auckland Hospital.”
Trevor and Jenny’s two children—two girls born only 18 months apart—both spent their earliest years living in London. Trevor was a supportive husband, who played an instrumental role in guiding Jenny with her career after motherhood.
“I was pregnant and I had to work because if you give up a whole year or eighteen months you’re absolutely stuffed for your career. You can’t do it again. So I had to be encouraged to work again, so he just pushed me out the door… Trevor pushed me out the door to go to work because he knew I had to have the training.”
Trevor sadly passed away from a brain tumour when he was only 42 years old, leaving Jenny to bring up their children, were aged only 10 and a half and 12 at the time. Competing against men without family commitments, Jenny never felt she had the option of working part-time and she feared her children may have resented her leaving them in the care of nannies while she worked long hours. However, it was because of her successful career that Jenny was able to provide educational opportunities for her children that she herself didn’t have.
Career: specializing in obstetrics and gynaecology
Despite her excellent performance in medical school and as a junior doctor, Jenny found it difficult to convince employers of her talents—both in England and later in New Zealand. She believed this to be a disadvantage of her gender and her role as a mother. She was forced to choose between obstetrics or gynaecology jobs, which did not count towards her O&G registration.
“I worked at Harefield Hospital and I couldn’t get jobs with O&G, both combined. I could only get gynaecological jobs—and that was not very good for your career… That was a terrible stigma, to have two children and be a woman… Nobody would employ me. Another overseas male doctor without my postgraduate qualifications got a job and I didn’t get it, it was terribly discriminatory.”
Not to be deterred, Jenny looked for another route into her chosen speciality. She went to the President of the Royal College of Obstetricians and Gynaecologists in London and asked him to support her job application, which allowed her to find work as an O&G registrar so that she could continue her training.
“I employed nannies to look after my kids. And there was no question that I was going to just give up. I was absolutely determined, and it was very, very difficult.”
After returning to New Zealand in 1968, Jenny found work as the tutor specialist in St Helen’s hospital—a public maternity hospital in Auckland that closed in 1990. This was a full-time position and Jenny was the first woman to be employed in this post. Over time, Jenny trained junior doctors and conducted research into perinatal mortality. Jenny’s career later expanded when she gained a combined O&G specialist role at National Women’s Hospital following the closure of St Helens.
Jenny had a very successful private O&G specialist for nearly 40 years delivering thousands of babies. Running her own practice was hard work, as she needed to find her own locums for time off, and she often relied on support from Dr John Thompson and Dr Neva Thakurdas.
Jenny also worked for the Family Planning Association in the 1970s and 1980s, including doing colposcopy, and also had a particular interest in intrauterine devices, stemming from the backlash against IUDs following the Dalkon Shield controversy. She published a long-term study of fertility in women who had received IUDs, in the American Journal of Obstetrics and Gynaecology which has been cited over 80 times.
Jenny was also instrumental in starting Contraceptive Choice, a group of women doctors who wanted to counteract misinformation about contraception. This group worked for 10 years producing evidenced based information to be used by GPs and FPA. She trained mid-career in laparoscopic surgery and after stopping obstetrics had a busy surgical career.
Retirement and thoughts about life
Although modest about her achievements, Jenny is proud that she was never one to back away from hard work, and it was this determination that allowed her to fight through any gendered challenges that stood in her way.
“I’m really contemptuous of a lot of women, they just don’t apply themselves to it. They have coffee mornings and they do a bit of medicine and then they give it up. And I’ve never liked that, I’ve always been a career woman who wanted to get on in life and learn as much as possible.”
Jenny retired from medical practice in 2009 when she was 74 years old. Jenny married her second husband Chris North who looked after her in her final years. She is survived by two daughters, Helen and Karen and five grandchildren.
“I got a lot out of my life. And my patients do love me actually, you’ll run across them sometimes. They really love me, and they really miss me and I miss them… I think the fact that I persevered, that’s the biggest achievement in my life. Nobody ever thinks their lives are good enough, do they?”
Speaking about today’s young doctors, Jenny feels strongly against organised strikes by house surgeons working in the hospital system, who demand better pay and working conditions. She agrees that the work is hard, although views it more as a rite of passage that must be endured.
“We worked harder than they work now, much harder… I just think that they’re very privileged people, to be doing medicine, and I just don’t agree with it.”
For those young women entering medicine today, Jenny has this advice for them.
‘Make certain that they put their career and their kids and family first!”
